What is Virus?
Novel Coronavirus Disease (Covid-19)
Cat: SCI
Pub: 2020
#2006b
Reports from WHO, ECDC, CDC, and ProSci
20406u
Title
Novel Coronavirus Disease 2019 (Covid-19)
新型コロナウイルス (Covid-19)
Index
Tag
; 2.4 vs 1.0; 14days; ACE2; Aetiology; Afebrile; Asymptomatic; CFR; ECMO; Incubation period; Infectivity; ; NIV; Pandemic; PPE; Prognosis; RCT; Respiratory tract; SARS-CoV-2; Severity; TESSy; Viral load; Viral RNA; Vital shedding;
Data
Why
- We have no effective ways to take countermeasure against the pandemic virus other than to take proper actions based on the fact-based knowledge accumulated from various global lessons and reports.
Original resume
Remarks
>Top 0. WHO declared pandemic
- WHO (World Health Organization) Director-General, Dr. Tedros Adhanom Ghebreyesus declares on 11 March 2020:
- Good afternoon. In the past two weeks, the number of cases of COVID-19 outside China has increased 13-fold, and the number of affected countries has tripled. There are now more than 118,000 cases in 114 countries, and 4,291 people have lost their lives. Thousands more are fighting for their lives in hospitals. In the days and weeks ahead, we expect to see the number of cases, the number of deaths, and the number of affected countries climb even higher. WHO has been assessing this outbreak around the clock and we are deeply concerned both by the alarming levels of spread and severity, and by the alarming levels of inaction.
- >Top We have therefore made the assessment that COVID-19 can be characterized as a pandemic. Pandemic is not a word to use lightly or carelessly. It is a word that, if misused, can cause unreasonable fear, or unjustified acceptance that the fight is over, leading to unnecessary suffering and death. Describing the situation as a pandemic does not change WHO’s assessment of the threat posed by this virus. It doesn’t change what WHO is doing, and it doesn’t change what countries should do.
- We have never before seen a pandemic sparked by a coronavirus. This is the first pandemic caused by a coronavirus. And we have never before seen a pandemic that can be controlled, at the same time. WHO has been in full response mode since we were notified of the first cases. And we have called every day for countries to take urgent and aggressive action. We have rung the alarm bell loud and clear.
- As I said on Monday, just looking at the number of cases and the number of countries affected does not tell the full story. Of the 118,000 cases reported globally in 114 countries, more than 90 percent of cases are in just four countries, and two of those – China and the Republic of Korea - have significantly declining epidemics. 81 countries have not reported any cases, and 57 countries have reported 10 cases or less.
- We cannot say this loudly enough, or clearly enough, or often enough: all countries can still change the course of this pandemic. If countries detect, test, treat, isolate, trace, and mobilize their people in the response, those with a handful of cases can prevent those cases becoming clusters, and those clusters becoming community transmission. Even those countries with community transmission or large clusters can turn the tide on this virus.
- Several countries have demonstrated that this virus can be suppressed and controlled. The challenge for many countries who are now dealing with large clusters or community transmission is not whether they can do the same – it’s whether they will. Some countries are struggling with a lack of capacity. Some countries are struggling with a lack of resources. Some countries are struggling with a lack of resolve.
- We are grateful for the measures being taken in Iran, Italy and the Republic of Korea to slow the virus and control their epidemics.
We know that these measures are taking a heavy toll on societies and economies, just as they did in China. All countries must strike a fine balance between protecting health, minimizing economic and social disruption, and respecting human rights. WHO’s mandate is public health. But we’re working with many partners across all sectors to mitigate the social and economic consequences of this pandemic.
- This is not just a public health crisis, it is a crisis that will touch every sector – so every sector and every individual must be involved in the fight. I have said from the beginning that countries must take a whole-of-government, whole-of-society approach, built around a comprehensive strategy to prevent infections, save lives and minimize impact.
- Let me summarize it in four key areas. First, prepare and be ready. Second, detect, protect and treat. Third, reduce transmission. Fourth, innovate and learn. I remind all countries that we are calling on you to activate and scale up your emergency response mechanisms; Communicate with your people about the risks and how they can protect themselves – this is everybody’s business; Find, isolate, test and treat every case and trace every contact; Ready your hospitals; Protect and train your health workers. And let’s all look out for each other, because we need each other.
- There’s been so much attention on one word. Let me give you some other words that matter much more, and that are much more actionable. Prevention. Preparedness. Public health. Political leadership. And most of all, people. We’re in this together, to do the right things with calm and protect the citizens of the world. It’s doable.
I thank you.
0. WHOパンデミック宣言:
- pandemic: disease prevalent over the world
- doable: feasible
- 2020/3/11 (大地震から9年目)
- 世界保健機構 (WHO)事務局長はCovid-19をパンデミックと宣言
- この日前の2習慣で、中国以外で感染者は、114カ国で11.8万人 (13倍)に拡大。
- WHOは、感染の拡大、重病化、無作為のリスクを警告する。
- Covid-19によるPandemicの宣言は初だが、各国がとるべき対応は変わらない。
- 感染の90%は、現在4カ国だが、この内、中国と韓国では感染が抑えられつつある。
- すべての国はpandemicとなるのを防ぐために、検査、処置、隔離、追跡およびこのために人材動員を図るべきである。
- 一部の国々では医療能力や人材不足が生じている。
- 現在、イラン、イタリー、韓国では感染が抑えられていることはありがい。中国でも、この抑制の対策のために社会や経済に多大の負担を生じた。
- これは公衆衛生にとっても危機だけではない。それは全ての分野や全ての個人にとっての闘いでもある。政府の全て、社会の全てでこれに対応しなければならない。
- 以下要点4項目を述べる。第一にはまず対応への準備、第二には、検査・保護・処置の実施、第三には感染拡大の減少、第四には創造力と教訓学習である。
- このウイルスのリスクについて情報交換し自身を守るよう呼びかける。これは全ての人の任務である。感染者の発見・隔離・検査・処置。医療機関と医療スタッフを守ること。相互による留意すること。
- さらに、感染防止、準備、公衆衛生、政治的リーダーシップ、とりわけ全ての人々に訴える。粛々と正しいことを実施して世界の市民を守ること。それは可能なことである。
Original resume
Remarks
>Top 1. Pandemic Covid-19: from ECDC report (12 March 2020)
- On 31 December 2019, a cluster of pneumonia cases of unknown aetiology was reported in Wǔhàn, Húběi Province, China. On 9 January 2020, China CDC reported a novel coronavirus as the causative agent of this outbreak, which is phylogenetically in the SARS-CoV. The disease associated with the virus is referred to as novel coronavirus disease 2019 (COVID-19).
- As of 11March 2020, 118, 598 cases of COVID-19 were reported worldwide by more than 100 countries. Since late February, the majority of cases reported are from outside China, with an increasing majority of these reported from EU/EEA countries and the UK.
- The Director General of the World Health Organization declared COVID-19 a global pandemic on 11 March 2020.
- All EU/EEA countries and the UK are affected, reporting a total of 17,413 cases as of 11 March. Seven hundred and eleven cases reported by EU/EEA countries and the UK have died. Italy represents 58% of the cases (n=10,149) and 88% of the fatalities (n=631). The current pace of the increase in cases in the EU/EEA and the UK mirrors trends seen in China in January-early February and trends seen in Italy in mid-February.
- In the current situation where COVID-19 is rapidly spreading worldwide and the number of cases in Europe is rising with increasing pace in several affected areas, there is a need for immediate targeted action. The speed with which COVID-19 can cause nationally incapacitating epidemics once transmission within the community is established, indicates that in a few weeks or even days, it is likely that similar situations to those seen in China and Italy may be seen in other EU/EEA countries or the UK.
- There are no vaccines available and there is little evidence on the effectiveness of potential therapeutic agents. In addition, there is presumably no pre-existing immunity in the population against the new coronavirus and everyone in the population is assumed to be susceptible. Clinical presentations of COVID-19 range from no symptoms (asymptomatic) to severe pneumonia; severe diseasecan lead to death. While the majority of cases (80%) are milder respiratory infections and pneumonias, severe illness and death is more commonamong the elderly with other chronic underlying conditions, with these risk groups accounting for the majority of severe disease and fatalities to date.
- The risk of severe disease associated with COVID-19 infection for people in the EU/EEA and UK is currently considered moderate for the general population and high for older adults and individuals with chronic underlying conditions, based on the probability of community transmission and the impact of the disease.
1. パンデミック Covid-19 (ECDC報告):
- aetiology: cause or manner of a desease, 病因学
- phylogenetic: 系統発生学
- EU/EEA: EEAは自由貿易協定
- therapeutic: 治療の
- asyptomatic: 自覚症状がない
- 2019/12/31河北省武漢市一体で感染病蔓延
- 2020/1/9には、新型コロナウイルスにより感染の爆発的増加発生
- 3/11には、世界100カ国で11.8万人に感染者が拡大。2月末以降の感染者の多数は中国以外の特に、欧州が多い。
- 3/11段階での欧州での感染者数は17千人。内、イタリーの感染者数は58%。ここまま推移すると欧州は1〜2月初の中国のような状況になる。
- Covid-19の感染力が強く、対象を絞った強力な対策が必須。爆発的感染は数週間〜数日中に発生する。
- 現在まだワクチンはなく、治療薬もなく、新型ウイルスなので免疫のある人もいない。
- 感染者は、80%は症状がないか軽微の症状だが、高齢者を中心に重篤・死亡に至る場合まである。
- 欧州での感染は、地域社会への感染としては、人口比ではまだ緩慢だが、高齢者層ではやや高い。
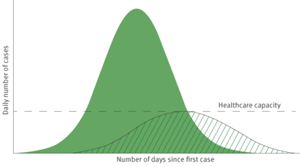
>Top 2. Symptom of the cases (ECDC):
- By 24 March 2020, 50,569 laboratory-confirmed cases have been reported to The European Surveillance System (TESSy).
- Information on symptoms was available for 14,011 cases from 13 countries, mainly (97%) from Germany. Among these cases, the most commonly reported clinical symptom was fever (47%), dry or productive cough (25%), sore throat (16%), general weakness (6%) and pain (5%). The frequency of these symptoms differs notably from those reported from China. Data on cases reported more recently to TESSy may be biased toward the more seriously ill because national policies have shifted focus towards testing of more severe cases.
- >Top Preliminary estimates of severity were based on the analysis of data from EU/EEA countries and the UK available in TESSy and online country reports (for countries whose data was incomplete or missing in TESSy).
- Among all cases:
- Hospitalisation occurred in 30% (13 122 of 43 438) of cases reported from 17 countries (median country-specific estimate, interquartile range (IQR): 24%, 11-41%)
- Severe illness (requiring ICU and/or respiratory support) accounted for 2 179 of 49 282 (4%) cases from 16 countries (median, IQR: 3%, 2-8%).
- Among hospitalised cases:
- Severe illness was reported in 15% (1 894 of 12 961) of hospitalised cases from 15 countries (median, IQR: 16%, 10-24%).
- Death occurred in 1 457 of 12 551 (12%) hospitalised cases from eight countries (median, IQR: 10%, 6-14%).
- Age-specific hospitalisation rates among all cases based on TESSy data showed elevated risk among those aged 60 years and above
- Robust estimates for case fatality risk for COVID-19 are still lacking and potentially biased by incomplete outcome data and differences in testing policies. The mean crude case-fatality (proportion of deaths among total cases reported) from the EU/EEA and the UK by 23 March 2020 was 5.4% (median country-specific estimate: 0.5%; range: 0.0-9.3%).
- >Top Based on a large dataset from cases in China, the overall case fatality risk (CFR) among laboratory-confirmed cases was higher in the early stages of the outbreak (17.3% for cases with symptom onset from 1-10 January) and has reduced over time to 0.7% for patients with symptom onset after 1 February. In data on diagnosed COVID-19 cases in China and South Korea, overall CFR was 2.3% and 0.5%, respectively, and increased with age in all settings, with the highest CRF among people over 80 years of age (14.8% and 3.7%, respectively). Similarly, age-specific estimates of crude case-fatality for Germany, Italy and Spain increased rapidly with age, particularly above 60 years of age. The absolute numbers of deaths also increased with age in each country: those aged 70–79 years accounted for 19% (Germany), 36% (Italy) and 20% (Spain) of all deaths per country; these proportions rose to 74% (Germany), 50% (Italy) and 67% (Spain) among those aged 80 years and above.
- >Top Data from a country report for Italy as of 19 March 2020 showed an increased risk of death among males compared with females in all age groups from 50 years and above. The risk of death becomes more pronounced with age, with an overall male-to-female ratio among COVID-19 deaths of 2.4:1. According to TESSy data from Germany as of 24 March 2020, this ratio is 1.6:1, with a particularly increased risk of death among males aged 70–79 years compared to their female contemporaries.
- >Top Among deceased patients in Italy until 19 March 2020, 73.8% had hypertension, 33.9% diabetes, 30.1% is chaemic heart disease, 22.0% atrial fibrillation, 19.5% a cancer diagnosed in the last five years. About half (48.6%) of the COVID-19 deaths had three or more comorbidities, 26.6% had two comorbidities, 23.5% had one comorbidity, and 1.2% had none. The most common complications observed in Italy were respiratory insufficiency (96.5%), acute kidney failure (29.2%), acute myocardial damage (10.4%) and bacterial superinfection (8.5%).
- >Top Incubation period:
- Current estimates suggest a median incubation period from five to six days for COVID-19, with a range from one to up to 14 days. A recent modelling study confirmed that it remains prudent to consider the incubation period of at least 14 days.
- Vital shedding:
- Over the course of the infection, the virus has been identified in respiratory tract specimens 1-2 days before the onset of symptoms and it can persist up to 8 days in moderate cases and up to 2 weeks in severe cases.
- >Top In terms of viral load profile, SARS-CoV-2 is similar to that of influenza, which peaks at around the time of symptom onset, but contrasts with that of SARS-CoV, which peaks at around 10 days after symptom onset, and that of MERS-CoV which peaks at the second week after symptom onset.
- Older age has also been associated with higher viral loads. The high viral load close to symptom onset suggests that SARS-CoV-2 can be easily transmissible at an early stage of infection.
- >Top Viral RNA has been detected in faeces from day 5 after symptom onset and up to 4 to 5 weeks in moderate cases, as well as in whole blood, serum, saliva and urine. Prolonged viral RNA shedding has been reported from nasopharyngeal swabs (up to 37 days among adult patients) and in faeces (more than one month after infection in paediatric patients). It should be noted that viral RNA shedding does not equate with infectivity.
- The viral load can be a potentially useful marker for assessing disease severity and prognosis: a recent study indicated that viral loads in severe cases were up to 60 times higher than in mild cases.
- >Top Basic reproduction number (R0):
- Recent modelling of the basic reproductive number (R0) from Italy estimates R0 between 2.76 and 3.25. Researchers from Lombardy who analysed the early phase of the outbreak in their region reported a reduction in R0 shortly after the introduction of mitigation measures.This is consistent with findings from China. A recent review of 12 modelling studies reports the mean R0 at 3.28, with a median of 2.79. Further research is needed to get a more accurate estimate of R0 in the various outbreak settings.
- >Top Infection in asymptomatic individuals:
- Asymptomatic infection at time of laboratory confirmation has been reported from many settings; a large proportion of these cases developed some symptoms at a later stage of infection. There are, however, also reports of cases remaining asymptomatic throughout the whole duration of laboratory and clinical monitoring.
- Viral RNA and infectious virus particles were detected in throat swabs from two German citizens evacuated from Hubei province on 1 February 2020 who remained well and afebrile seven days after admission to a hospital in Frankfurt.
- A mother and her child (from a family cluster) who both tested positive by quantitative RT-PCR (nasopharyngeal swab samples) remained asymptomatic (including normal chest CT images during the observation period).
- Similar viral loads in asymptomatic versus symptomatic cases were reported in a study including 18 patients. Persistent positivity of viral RNA in throat and anal swabs was reported in an asymptomatic female patient after 17 days of clinical observation and treatment.
- Transmission in pre-symptomatic stage of infection:
- No significant difference in viral load in asymptomatic and symptomatic patients has been reported, indicating the potential of virus transmission from asymptomatic patients. Major uncertainties remain with regard to the influence of pre-symptomatic transmission on the overall transmission dynamics of the pandemic because the evidence on transmission from asymptomatic cases from case reports is suboptimal.
- Pre-symptomatic transmission has also been inferred through modelling, and the proportion of pre-symptomatic transmission was estimated between 48% and 62%. Pre-symptomatic transmission was deemed likely based on a shorter serial interval of COVID-19 (4.0 to 4.6 days) than the mean incubation period (five days). The authors indicated that many secondary transmissions would have already occurred at the time when symptomatic cases are detected and isolated.
- Children:
- Children made up a very small proportion of the 50,068 cases reported to TESSy as of 24 March (with known age (<10 years (1%), 10–19 years (4%)). The male-to-female ratio (1.2:1 overall) was less pronounced in children (1.1 and 1.0 in those aged 10–19 and <10 years, respectively) and increased with age. The age distribution observed in the EU/EEA and the UK reflects testing policies and case definitions, which usually include symptoms, and it is possible that the small proportion of affected children reflects a lower risk of children to develop COVID-19. Current literature indicates that children are as likely to be infected as adults but they experience mild clinical manifestations. Data in TESSy show no difference between age groups in the order of most common symptoms but fever was slight less commonly reported among those aged 10–19 years of age (39%, compared to 47% for all ages) and sore throat was less common among those aged <10 years (10%, compared to 16% for all ages). Asymptomatic cases in infants and children have been also reported. Two studies on patients with positive laboratory results reported that 10/15 (66.7%) and 4/31 (13%) of the children were asymptomatic. Exposure to COVID-19 among children is likely to occur within the family or in a household context.
- Pregnant women and neonates:
- >Top Pregnant women appear to experience similar clinical manifestations as non-pregnant adult patients with COVID-19 pneumonia. There are only two reported cases of mothers with ICU admission and requiring mechanical ventilation or extracorporeal membrane oxygenation (ECMO). No maternal deaths have been reported so far. COVID-19 appears to be less lethal for pregnant women than SARS (15% CFR in pregnancy) and MERS (27% CFR in pregnancy). There is limited evidence of severe adverse outcomes, such as miscarriage, preterm birth, stillbirths and foetal distress. No pregnancy losses and only one stillbirth have been reported to date. Intrauterine transmission appears to be unlikely. Elective Caesarean section deliveries have been commonly reported as a precautionary method to avoid perinatal transmission. A confirmed COVID-19 neonatal case has been recently reported, however the mode of transmission remains unclear. A neonate born to a confirmed maternal case had negative laboratory results for COVID-19 and died due to multi-organ failure. The virus has not been found in breastmilk.
- Vulnerable groups:
- Data from Italy corroborate previously identified population groups at higher risk for having severe disease and death. These groups are elderly people above 70 years of age, and people with underlying conditions such as hypertension, diabetes, cardiovascular disease, chronic respiratory disease and cancer. Men in these groups appear to be at a higher risk than females. Chronic obstructive pulmonary disease (COPD), cardiovascular diseases, and hypertension have been identified as strong predictors for ICU admission.
- Higher ACE2 (angiotensin converting enzyme II) gene expression may be linked to higher susceptibility to SARS-CoV-2. It has been shown that ACE2 expression in lung tissues increases with age, tobacco use and with some types of antihypertensive treatment. These observations might explain the vulnerability of older people, tobacco users/smokers and those with hypertension; they also highlight the importance of identifying smokers as a potential vulnerable group for COVID-19.
- Immunity:
- It is too early to know how long the protective immune response against SARS-CoV2 will last, as this will require longitudinal serological studies that follow patients’ immunity over an extended period of time. Evidence from other coronavirus infections (SARS and MERS) indicates that immunity may last for up to three years and re-infection with the same strain of seasonal circulating coronavirus is highly unlikely in the same or following season. This could also hold true for SARS-CoV2 as there is emerging evidence from early studies suggesting that that individuals develop antibodies after infection and are likely to be immune from reinfection in the short term.
- Seasonality:
- The four coronaviruses that are endemic in human populations are responsible for 10–15% of common cold infections and display a marked winter seasonality in temperate climates, with a peak between December and April, but are hardly detected in the summer months. The seasonality of coronaviruses might be driven, in part, by environmental conditions and host susceptibility, because coronaviruses are more stable under low and midrange relative humidity (20–50%) when the defence mechanisms of the airways are suppressed. However, based on preliminary analyses of the COVID-19 outbreak in China and other countries, high reproductive numbers were observed not only in dry and cold districts but also in tropical districts with high absolute humidity, such as in Guangxi and Singapore. There is no evidence to date that SARS-CoV-2 will display a marked winter seasonality, such as other human coronaviruses in the northern hemisphere, which emphasises the importance of implementing intervention measures such as isolation of infected individuals, workplace distancing, and school closures.
- Survival in the environment:
- Recent publications have evaluated the survival of SARS-CoV-2 on different surfaces. The environmental stability of viable SARS-CoV-2 is up to 3 hours in the air post aerosolisation, up to 4 hours on copper, up to 24 hours on cardboard, and up to 2–3 days on plastic and stainless steel, albeit with significantly decreased titres. These findings are comparable with the results obtained for environmental stability of SARS-CoV-1. However, as these are results from experimental studies, they do not directly translate to fomite infectivity in the real world.
- Different levels of environmental contamination have been described in rooms of COVID-19 patients, ranging from 1 positive out of 13 samples to 13 out of 15 samples testing positive for SARS-CoV-2 before cleaning. No air samples were positive in these studies, but one sample from an air exhaust outlet was positive indicating, according to the authors, that virus particles may be displaced by air and deposited on surfaces.
- In a study of environmental contamination in a Chinese hospital during the COVID-19 outbreak, SARS-CoV-2 was detected in environmental samples from intensive care units (ICU) dedicated to COVID-19 care, a COVID-19-dedicated obstetric isolation ward, and a COVID-19-dedicated isolation ward. SARS-CoV-2 was also detected on objects such as the self-service printers used by patients to self-print the results of their exams, desktop keyboards and doorknobs. Virus was detected most commonly on gloves (15.4% of samples) but rarely on eye protection devices (1.7%). This evidence indicates that fomites may play a role in transmission of SARS-CoV-2 but the relative importance of this route of transmission compared to direct exposure to respiratory droplets is still unclear.
- >Top Treatment:
- There is currently no approved specific treatment or vaccine against COVID-19 infection. Patients require supportive care and oxygen supplementation. This can be done through NIV (non-invasive ventilation; if performed in a negative pressure room or through a helmet) or via mechanical ventilation. Critically ill patients may also require vasopressor support and antibiotics for secondary bacterial infections. Clinician reports from Italy and the USA refer to a number of complications such as cardiomyopathy and sudden onset death, as well as thromboembolic episodes (pulmonary embolism). Data collection through the World Health Organization’s COVID-19 Clinical Network is ongoing to assess the frequency of these complications.
- >Top A number of pharmaceuticals are being used for severe and critically ill patients as potential treatments against SARS-CoV-2, including ribavirin, interferon β-1a, the antiviral combination lopinavir/ritonavir, the antimalarial chloroquine/hydroxychloroquine, the antiviral nucleotide analogue remdesivir and the antiviral favipiravir. It is important that the available pharmaceuticals are carefully assessed in randomised controlled trials (RCTs); several clinical trials are recruiting patients globally to assess the effect of different treatment options.
- A randomised, controlled, open-label trial of lopinavir/ritonavir in 199 COVID-19 patients in China failed to show any favourable effect on the clinical course or the mortality compared to standard treatment. Hydroxychloroquine has been shown in vitro to alter the uptake of the virus in cells, and a small case series and trial have reported its use in patients during this outbreak in China and Europe. It remains one of the possible therapies that needs to be evaluated through an adequately sized RCT.
- Systemic use of steroids is not recommended because they might increase the viral replication and shedding of the virus along with other steroid-related side effects. Other approaches are also assessed such as the blocking of the inflammatory cascade by IL6- & IL4- blockers.
- >Top Reports that non-steroidal anti-inflammatory drugs worsen COVID-19 through increased expression of angiotensin-converting enzyme 2 (ACE2), whose receptor is used by SARS-CoV-2 to enter the target cells, are not supported by evidence.
1. 感染者の症状 (ECDC報告):
- TESSy: The European Surveillance System
- atrial fibrillation: 心房細動
- comorbidities: 併存症
- respiratory tract:
- faeces: 排泄物
- neonate: 新生児
- ECMO: 体外式膜型人工肺
- miscarriage: 流産
- stillbirth: 死産
- foetal distress: 仮死
- NIV: non-invasive intermittent ventilation, 非侵襲的換気療法 (陽圧式と陰圧式を含む; )
- NIPPV: non-invasive postive pressure ventilation, 非侵襲的陽圧換気療法
- vassopressor: 昇圧薬
- RCT: randomized controlled trial ランダム化比較対照試験 (治療する介入群と、治療しない対照群に分けて比較試験を行う)
- ACE2: ウイルスはACE2を、宿主細胞受容体として利用し、ACE2の発現を低下させ、急性配布前などの重大な症状を引き起こす。
- 欧州での患者数 (2020/3/14時点)
- 欧州での感染者数は50.5千人
- 14,011事例での感染症状は、発熱(47%), 痰咳 25%, 咽喉炎 16%, 体力低下 6%, 痛み 5%。データがより深刻になっているのは、重症者中心の検査による。
- 欧州での重症患者:
- 欧州17カ国入院患者 30%、重症患者4%
入院患者の内、重症患者比率15%、死亡12%。60歳以上の患者のリスクは高い。
- まだデータとしては不十分。3/23現在の重症化率(CFR) 5.4%
- 中国・韓国での重症化率
- 1/1-10の間は17.3%だったが、2/1以降は0.7%に低下
- 全体として、中・韓での重症化率はそれぞれ2.3%と0.5%。但し、80歳以上の場合はそれぞれ14.8%と3.7%になる。
- Report of WHO-China Joint Mission (24 Feb 2020)
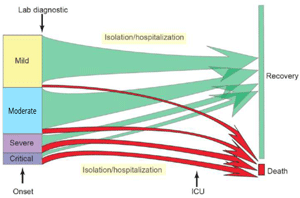
- 男女感染比率:
- 欧州でも、重症化率は50歳以上で男性の比率が女性より2.4倍と高い。
- 患者の過去の既往症との関係では、 Covid-19による死亡の場合、高血圧、糖尿病、癌などとの3既往患者は約50%、2既往は26.6%、1既往は23.5%、既往歴がない場合は1.2%
- このCovid-19が発症する合併症は、イタリーでは、併発患者は、呼吸不全 96.5%、急性腎不全 29.2%、急性心筋障害 10.4%、細菌重複感染 8.5%
- 潜伏期間:
- Covid-19の場合 5-6日から14日まであるので、安全度としては14日間
- ウイルス生存:
- 感染期間を通じて、ウイルスは、発症まで1-2日滞留し、軽症では8日間、重症では14日間滞在。
- ウイルス量の経過で見ると、SARS-CoV-2はインフルエンザに似ていて、宿主が発症時がピークだが、SARS-CoVではそれと異なり、発症後10日頃ピークとなり、MERS-CoVは、発症後2週間がピークとなる。
- 高齢者はこのピーク時が関係する。発症時がピークということは、SARS-CoV-2は、感染の早い時期に容易に伝染しやすいということである。
- ウイルスRNA:
- ウイルスのRNAは、発症後5日から通常の感染の場合4-5週間の間に、全血、血清、唾液、尿中に検知される。
- ウイルスが長期間生存する場合、成人の鼻咽頭の綿棒から37日後まで、また小児患者の場合はその排泄物から1ヶ月後にも得られるとの報告がある。RNAの生存期間とウイルスの感染力には相関関係がない。
- ウイルス量は、感染症の重篤度や予後診断を評価する指標となり得る。重篤の場合は、軽症の場合の60倍という研究結果もある。
- 1感染者当たりの2次感染者数 (R0):
- イタリーの場合は、2.76〜3.25である。Lombardyでは、感染緩和策の導入後は、このR0は、中国の場合と同様に減少した。最近の調査ではこのR0は3.28で、中位数は2.79である。今後更に正確なR0を研究する必要がある。
- 無発症の感染者:
- 実験室あるいは臨床現場で、感染の後期にこの無発症の患者が報告されている。
- 2/1に河北省から退避してきた2名のドイツ人は、Frankfurtで入院後、喉綿棒で陽性を確認したが、7日間は発熱なし。
- 鼻咽頭綿棒検査で陽性だった母子も、胸部CT検査中も発熱はなかった。
- 同様に18名の感染者に関して、症状ありとなしの場合のウイルス量の検査が行われれいる。この間、喉と肛門の綿棒検査で陽性だった女性も、受診後17間も発症していない。
- 感染の発症前段階での伝染性:
- 発症の有無によるウイルス量に大きな違いはないので、発症していない感染者からも伝染の可能性がある。Pandemicの場合、非発症者からどのように感染していくのかまだ不確実である。
- 発症前の感染は、モデル計算によって48%〜62%とされている。発症前感染はおそらく平均潜伏期間5日よりも短く、Covid-19の短い方の連続感染間隔(4.0〜4.6日)ではないかと予測されている。感染者が発症する時点ではすでに多くの二次感染が発生しているのではないかと思われる。
- 子供
- 子供の発症は、3/24現在、50千例と少ない (10歳未満1%、10-19歳4%)。男女比は1.2対1で、年齢上昇に伴い増加傾向。子供も同様に感染するが、発症例は少ない。発症した場合でも、症状での年齢差は特にないものの発熱する割合はやや低い (10-19歳39%、全体では16%)。幼児や子供で非発症も報告されている。おそらく家庭内感染であろう。
- 妊婦・新生児:
- 妊婦の発症状況は、非妊婦の場合と同様である。現在ICUでECMO(体外式膜型人工肺) が必要な2例が報告されている。死亡例は、妊婦の死亡例は、Covid-19の場合はないが、SARSの場合の致命率(CFR)は、15%, MERSの場合27%だった) 。流産・死産・仮死産のような重篤な結果となる事例は限られている。今日までに流産はなく、死産が1例だけある。新生児の感染は最近報告されたが、感染経路は不明である。。新生児は、陰性の妊婦から誕生したものの多臓器不全で死亡した。なお、母乳からはウイルスは発見されていない。
- ウイルスに脆弱な集団:
- イタリーの事例では、70歳以上の高齢者で、高血圧、糖尿病、心血管疾患、慢性呼吸器疾患、癌を伴う人。女性よりも男性がリスクが高い。慢性閉塞性肺疾患、心血管疾患、高血圧患者はICU治療の予備軍とされる。高齢者、喫煙者、高血圧者もCovid-19にとっては脆弱なグループと言える。
- 免疫:
- SARS-CoV2(Covid-19の原因ウイルス名)の場合は、感染後抗体が生成され、短期間での再感染からの免疫となることが知られているが、それがいつまで継続できるのかもまだ決定的ではない。
- 季節性:
- 4つのコロナウイルスは、一般的な風邪の10-15%に感染を引き起こし、冬季(12月〜4月まで) にピークを迎え、夏期にはほぼ検知されない季節性がある。コロナウイルスは、気道の防御機構が抑制されている場合、低中湿度(20-50%)でより安定的となる。中国などでのCovid-19の感染爆発の分析では、低温乾燥だけでなく、江西省やSingaporeなど高温多湿でも感染が確認されている。
- SARS-CoV-2に冬季中心という季節性の証拠はまだない。現在は北半球で、隔離、離間、学校閉鎖など感染防止の対策に注力している最中である。
- 環境でのウイルスの生存:
- SARS-CoV-2ウイルスは、エアロゾル中で3時間、銅金属上で4時間、段ボール上で24時間、プラスチックやステンレス上で2-3日間、若干弱まるが生存する。これらはSARS-CoV-1の場合と同様である。但し、これらは実験室レベルでの結果であって、実際の感染での結果ではない。
- Covid-19の患者の部屋での様々な環境汚染状態の報告されており、13サンプルの内1サンプルから15サンプルの内13サンプルまで陽性だった。ウイルス粒子は空気中を移動して、表面に堆積すると見られる。
- Covid-19感染爆発の期間中の中国での環境調査によれば、SARS-CoV-2は、ICUや産科隔離病棟でも発見されている。また、患者が使用するプリンタ、キーボード、ドアノブなどからも、またウイルスは手袋(15.4%)、眼球保護用具(1.7%)からも検出された。これは呼吸飛沫への直接接触に比べて、何かを媒介して感染する場合より重要なのかはまだ明らかではない。
- 治療:
- 現在まだCovid-19感染に対する承認された特定の治療やワクチンはまだない。患者には、支援療法と酸素補給となる。これはNIV装置による。
- 重篤患者は昇圧薬と抗生物質を投与して二次的最近感染を防ぐ必要がある。イタリーや米国での臨床報告では、心筋症や突然死、血栓塞栓症 (肺塞栓症)などの合併症を起こしている。現在、WTOのCovid-19による臨床ネットワークによるデータ収集を行っている。
- 現在SARS-CoV-2の重症患者に対する治療薬としては、1) ribavirin, 2) interferon β-1a, 3) antiviral combination lopinavir/ritonavir, 4) antimalarial chloroquine/hydroxychloroquine, 5) antiviral nucleotide analogue remdesivir および 6) antiviral favipiravirである。治療薬の効果は、RCT (ランダム化比較対照試験) で慎重に行う必要がある。
- 中国での199人の患者に対するlopinavir/ritonavirのRCT試験では、治療効果や死亡率について有意の結果は得られなかった。Hydroxychloroquineは、ウイルスの細胞侵入を変化させるとの実験室で示されており、中国や欧州での感染爆発時での使用が報告されている。現在はまだ、ある規模でのRCTを通じた評価が必要な治療法の一つに留まっている。
- ステロイドの全身使用は、ウイルスの複製と排出を増加させ、また他ステロイドの副作用もあるので推奨されない。 IL6- & IL4- blockerによる炎症の連続を遮断することも評価中である。
- 非ステロイド性抗炎症薬は、Angiotensin変換酵素2 (ACE2)の発現増加を通じてCovid-19を悪化させるとの報告は、その受容体がSARS-CoVによって標的細胞に侵入するために利用されているという点は、まだ証拠は明らかではない。
>Top 3. Outbreak stages: Annex: Scenarios to describe progression of COVID-19 outbreaks
- The following five scenarios, adapted from ECDC’s strategic analysis, are used to describe the possible progression of the COVID-19 outbreak in EU/EEA countries.
- Scenario-0:
- describes a situation with no reported cases in the country and multiple introductions and/or community transmission elsewhere in Europe. At this stage, the main objective for public health measures should be to enable rapid detection and isolation of individual cases to prevent domestic transmission chains, and to prepare for the response once cases are detected in the country.
- Scenario-1:
- describes a situation with multiple introductions but limited local transmission in the country. Despite the introductions there is no apparent sustained transmission (only second generation cases observed or transmission within sporadic contained clusters with known epidemiological links). In this situation, the objective is containment of the outbreak by blocking transmission opportunities, through early detection of imported and locally-transmitted COVID-19 cases in order to try to avoid or at least delay the spread of infection and the associated burden on healthcare systems. Delaying the start of local transmission will allow the current influenza season to end, freeing up some healthcare capacity.
- Scenario-2:
- >Top describes a situation with increasing number of introductions and of more widespread reports of localised human-to-human transmission in the country (more than two generations of cases outside of sporadic clusters with known epidemiological links). In this situation, the objective remains to contain where practicable and otherwise slow down the transmission of the infection. This will increase the time available for development, production and distribution of PPE and effective therapeutic options, and would play a crucial role in reducing the burden on the healthcare system and other sectors, particularly if wider transmission of COVID-19 is delayed beyond the ongoing influenza season. A reduced burden would also allow for more time to increase laboratory capacity, and increase surge capacity in healthcare services. All these measures will facilitate effective treatment of infected patients[44]. Rapid collection and analysis of epidemiological and virological data will enable targeting of measures in this scenario and later.
- Scenario-3:
- describes a situation with localised outbreaks, which start to merge becoming indistinct. In this scenario, there is sustained human-to-human transmission in the country (more than two generations of cases outside of sporadic clusters with known epidemiological links) and an increasing pressure on health care systems. The objective at this stage is to mitigatethe impact of the outbreak by decreasing the burden on health care systems and protect populations at risk of severe disease. At the same time, operational research should guide developing better and more efficient diagnostic and treatment options.
- Scenario-4:
- describes a situation with widespread sustained transmission where healthcare systems are over-burdened due to a large demand for emergency healthcare services, a strained ICU capacity, overworked healthcare workers and reduced staff availability due to illness, lack of PPE and lack of diagnostic testing capacity. The objective at this stage is still to mitigate the impact of the outbreak, decrease the burden on healthcare services, protect populations at risk of severe disease and reduce excess mortality.
3. 感染爆破の諸段階:
- PPE: personal protective equipment 個人防護具
- surge capacity: 急増・沸騰への対応能力
- 欧州でのCovid-19の感染状況についての戦略的な分析による5段階:
- シナリオ-0:
- 欧州内での他の国・地域への複数の感染事例の報告にまだ至っていない状況。この段階での、公衆衛生の主な目的は、迅速な検査と個々の感染者の隔離によって国内感染連鎖を阻止し、国内での感染事例に対する準備を行うこと。
- シナリオ-1:
- 複数の感染が発生しているものの国内の局所限定的な感染に留まっている状況。その感染がまだ連鎖している明らかな状況ではない場合 (または既知の疫学的リンクのある散発的な感染クラスターの内部で2世代のみの感染症例が確認された状況) この状況での目的は、感染機会を遮蔽することで、インポートされ局所的に発生した感染の早期検出によって、感染拡大と医療システムの負担回避あるいは少なくとも負荷軽減させる。地域での伝染を遅らせることで、現在のインフルエンザ流行期を終わらせ、一部の医療余力を開放する。
- シナリオ-2:
- 国内での局所的な人対人の感染の増加が広く報告が増えている状況。 (既知の疫学的リンクのある散発的クラスターの外側に2世代超の感染症例) この状況での目的は、引き続き実行可能な方法で感染の遅延化を図ることである。これはPPEおよび治療方法の開発・生産・配布に必要な時間を増やす、また、医療機関等他部門への負担軽減は、より広範な感染を遅らせ、現在のインフルエンザ流行期間を超える場合には特に重要になる。負担軽減はさらに検査能力や医療機関の対応能力を増やす時間を確保する。これらの対策によって、患者への効果的な処置が容易になる。疫学的・ウイルス学的データの迅速な収集と分析により今後のシナリオへの対応を絞ることができる。
- シナリオ-3:
- 局所的なアウトブレイクが発生し、それが合体始めたのか不明であるような状況。この局面では、国内で人対人の感染がある。 (既知の疫学的リンクのある散発的クラスターの外側に2世代超の感染症例) さらに医療システムへの圧力が増加している。この段階での目的は、医療システムへの負荷軽減することでアウトブレイクの影響を軽減し、重篤化するリスク集団を保護することである。同時に、統計的な処理 (OR) によってより優れてかつ効果的な診断・治療のオプションの開発を先導すべきである。
- シナリオ-4:
- 持続的な感染が広範囲に及んでおり、緊急利用サービスへ、ICU収容能力、医療従事者の過労や病気による要因減、PPEや診断検査能力の不足等による、巨大な需要に発生で医療システムには過大な負担がかかっている状況。この段階での目的は、アウトブレイクへの影響を軽減し、医療機関への負担を減らし、病気の重篤化リスク集団を保護し、過剰な死亡率を減少させることである。
>Top 4. Advices from WHO: Myth busters
- Covid-19 virus can be transmitted in areas with hot and humid climates:
- From the evidence so far, the COVID-19 virus can be transmitted in ALL AREAS, including areas with hot and humid weather. Regardless of climate, adopt protective measures if you live in, or travel to an area reporting COVID-19. The best way to protect yourself against COVID-19 is by frequently cleaning your hands. By doing this you eliminate viruses that may be on your hands and avoid infection that could occur by then touching your eyes, mouth, and nose.
- Cold weather and snow CANNOT kill the new coronavirus:
- There is no reason to believe that cold weather can kill the new coronavirus or other diseases. The normal human body temperature remains around 36.5°C to 37°C, regardless of the external temperature or weather. The most effective way to protect yourself against the new coronavirus is by frequently cleaning your hands with alcohol-based hand rub or washing them with soap and water.
- Taking a hot bath does not prevent the new coronavirus disease
- Taking a hot bath will not prevent you from catching COVID-19. Your normal body temperature remains around 36.5°C to 37°C, regardless of the temperature of your bath or shower. Actually, taking a hot bath with extremely hot water can be harmful, as it can burn you. The best way to protect yourself against COVID-19 is by frequently cleaning your hands. By doing this you eliminate viruses that may be on your hands and avoid infection that could occur by then touching your eyes, mouth, and nose.
- The new coronavirus CANNOT be transmitted through mosquito bites.
- To date there has been no information nor evidence to suggest that the new coronavirus could be transmitted by mosquitoes. The new coronavirus is a respiratory virus which spreads primarily through droplets generated when an infected person coughs or sneezes, or through droplets of saliva or discharge from the nose. To protect yourself, clean your hands frequently with an alcohol-based hand rub or wash them with soap and water. Also, avoid close contact with anyone who is coughing and sneezing.
- Are hand dryers effective in killing the new coronavirus?
- No. Hand dryers are not effective in killing the 2019-nCoV. To protect yourself against the new coronavirus, you should frequently clean your hands with an alcohol-based hand rub or wash them with soap and water. Once your hands are cleaned, you should dry them thoroughly by using paper towels or a warm air dryer.
- Can an ultraviolet disinfection lamp kill the new coronavirus?
- UV lamps should not be used to sterilize hands or other areas of skin as UV radiation can cause skin irritation.
- How effective are thermal scanners in detecting people infected with the new coronavirus?
- Thermal scanners are effective in detecting people who have developed a fever (i.e. have a higher than normal body temperature) because of infection with the new coronavirus.
- However, they cannot detect people who are infected but are not yet sick with fever. This is because it takes between 2 and 10 days before people who are infected become sick and develop a fever.
- Can spraying alcohol or chlorine all over your body kill the new coronavirus?
- No. Spraying alcohol or chlorine all over your body will not kill viruses that have already entered your body. Spraying such substances can be harmful to clothes or mucous membranes (i.e. eyes, mouth). Be aware that both alcohol and chlorine can be useful to disinfect surfaces, but they need to be used under appropriate recommendations.
- Do vaccines against pneumonia protect you against the new coronavirus?
- No. Vaccines against pneumonia, such as pneumococcal vaccine and Haemophilus influenza type B (Hib) vaccine, do not provide protection against the new coronavirus.
- The virus is so new and different that it needs its own vaccine. Researchers are trying to develop a vaccine against 2019-nCoV, and WHO is supporting their efforts.
- Although these vaccines are not effective against 2019-nCoV, vaccination against respiratory illnesses is highly recommended to protect your health.
- Can regularly rinsing your nose with saline help prevent infection with the new coronavirus?
- No. There is no evidence that regularly rinsing the nose with saline has protected people from infection with the new coronavirus.
- There is some limited evidence that regularly rinsing nose with saline can help people recover more quickly from the common cold. However, regularly rinsing the nose has not been shown to prevent respiratory infections.
- Can eating garlic help prevent infection with the new coronavirus?
- Garlic is a healthy food that may have some antimicrobial properties. However, there is no evidence from the current outbreak that eating garlic has protected people from the new coronavirus.
- Does the new coronavirus affect older people, or are younger people also susceptible?
- People of all ages can be infected by the new coronavirus (2019-nCoV). Older people, and people with pre-existing medical conditions (such as asthma, diabetes, heart disease) appear to be more vulnerable to becoming severely ill with the virus.
- WHO advises people of all ages to take steps to protect themselves from the virus, for example by following good hand hygiene and good respiratory hygiene.
- Are antibiotics effective in preventing and treating the new coronavirus?
- No, antibiotics do not work against viruses, only bacteria.
- The new coronavirus (2019-nCoV) is a virus and, therefore, antibiotics should not be used as a means of prevention or treatment.
- However, if you are hospitalized for the 2019-nCoV, you may receive antibiotics because bacterial co-infection is possible.
- Are there any specific medicines to prevent or treat the new coronavirus?
- To date, there is no specific medicine recommended to prevent or treat the new coronavirus (2019-nCoV).
- However, those infected with the virus should receive appropriate care to relieve and treat symptoms, and those with severe illness should receive optimized supportive care. Some specific treatments are under investigation, and will be tested through clinical trials. WHO is helping to accelerate research and development efforts with a range or partners.
6. WHOからの勧告:
- mucous: 粘液の
- pneumonia: 肺炎
- co-infection: 同時感染
- Covid-19ウイルスは、高温多湿でも伝染する:
- 今までの事例では、高温多湿気候を含め全ての地域で伝染する。従って、Covid-19感染地域への居住・旅行には感染予防が欠かせない。頻繁に手洗いをすることで、目・口・鼻への接触感染を防止することができる。
- 寒気や積雪はウイルスを死滅させない:
- 寒気が新型ウイルスを死滅されるとの証拠はない。人間の平温は外部の温度にかかわらず、36.5〜37ºCである。最も効果的なのは、石鹸を使ったこすり手洗いとアルコール消毒である。
- 高温の風呂でもウイルスは防げない:
- 高温の風呂でもウイルスの感染は防げない。高温シャワーを浴びても体温は36.5〜37ºCで変わらない。むしろあまりにも高温の風呂は、やけどの可能性もあり、体にはむしろ有害。Covid-19を感染を防ぐには、こまめな手洗い励行と目口鼻を触らないことである。
- ウイルスは蚊からは媒介されない:
- 今までウイルスが蚊で媒介された例は報告されていない。新型ウイルスは、感染した人の咳やくしゃみで発生する飛沫、または唾液や鼻からの飛沫を通じて主に感染する呼吸器ウイルスである。これらを防ぐには、頻繁な石鹸を使った手洗いとアルコール消毒。また、咳やくしゃみをしている人との接触を避けることが重要。
- ハンドドライヤーはウイルスを殺すか:
- ノー。ハンドドライヤーはCovid-19を殺さない。頻繁な手洗いとアルコール消毒が有効である。手洗いをした後、ペーパータオルまたは温かいドライヤーで乾燥させるのが良い。
- 紫外線はウイルスを殺すか:
- UVランプは、手や他の部分の殺菌消毒はしないで下さい。皮膚の炎症を起こす可能性がありますので。
- サーマルスキャナーはコロナウイルスの検知にはどの程度有効か:
- サーマルスキャナーは、ウイルスにかかって通常より高熱の症状がある場合は有効である。
- 但し、ウイルスに感染したものの発熱症状がない人は検知できない。これは感染したがまたは発熱を伴う発症が起きていない状態で、通常発熱症状までに2-10日かかるからである。
- アルコールや塩素を全身に振りかけるとウイルスは死滅するか:
- ノー。全身にアルコールや塩素をふりかけてもウイルスはすでに身体に侵入しているので殺せない。むしろ衣服や粘膜 (目や口)に有害である。アルコールや塩素は、表面の少ドックには役立つが、適切な指導の下に使用する必要がある。
- 肺炎に対するワクチンは、新型ウイルスにも効くか:
ノー。肺炎に対するワクチン (肺炎球菌ワクチン、ヘモフィルス・インフルエンザB型 (Hib)ワクチン等) は新型ウイルスに対して効果はない。
- このウイルスは新型で異なるので、それ独自のワクチンが必要となる。研究者は現在、2019-nCovに対するワクチンを開発中で、WHOもそれを支援している。
- 2019-nCoVに対しては効果はないものの、呼吸器疾患に対するワクチンは保健としての効果はある。
- 生理食塩水で鼻をすすぐと、新型ウイルス防止に効果があるか:
- ノー。そのような効果は証明されていない。
- 但し、いつもそのように生理食塩水で鼻をすすぐ通常の風邪を早く治す意味で一定の効果はある。但し、これをやっても呼吸器感染症を予防することにはならない。
- ニンニクを食べると新型ウイルス予防効果はあるか:
- ノー。ニンニクはある種の抗菌特性をもつ健康食品であるが、新型ウイルスを食することで現在の大発生を予防できるとの証拠はない。
- 新型ウイルスは高齢者に感染するか、それとも若い人に感染するか:
- 新型ウイルス(2019-nCoV)に感染するので全ての年齢の人々である。高齢者でかつ既往の病状 (喘息、糖尿病、心臓病など) がある場合は、このウイルスにより病状が重症化となる傾向がある。
- WHOは、全ての盛大に対して、ウイルスに感染しないように、手と呼吸器の衛生によって身を守るように勧告している。
- 抗生物質は、新型ウイルスに対して効果があるか:
- ノー。抗生物質は、細菌に効果はあるが、ウイルスには効かない。
- 2019-nCoVはウイルスであるので、抗生物質は予防や治療の手段として使用すべきではない。
- しかし、2019-nCoVで入院した場合、細菌による同時感染があり得るので抗生物質を投与されることがあり得る。
- 新型ウイルスの予防や治療に効く特定の薬はあるか:
- 現在の所、新型ウイルス (2019-nCoV)の予防・治療の適する特定の薬は存在しない。
- しかし、そのウイルスに感染した患者は、症状を緩和したり治療するための適切なケアを受ける必要がある。また重症の人はさらに最適なケアを受けるべきである。具体的な治療は現在調査中で、今後臨床試験を通じてテストされる。WHOも広範なパートナーでこのR&Dの加速化を支援している。
>Top 5. Structiure of Covid-19 (ProSci)
- COVID-19 is an acute respiratory disease caused by novel coronavirus SARS-CoV-2 also known as 2019-nCoV. On March 11, 2020, the World Health Organization (WHO) characterized COVID-19 as a pandemic.
- >Top COVID-19 coronavirus SARS-CoV-2 belongs to the Betacoronavirus genus originating from bats. Betacoronaviruses can infect mammals, are zoonotic pathogens, and can cause severe respiratory disease in humans. Other viruses in this family are SARS coronavirus and MERS coronavirus. COVID-19 (SARS-CoV-2) has approximately 79% sequence identity to SARS-CoV and 50% to MERS-CoV. In addition, homology modeling shows COVID-19 (SARS-CoV-2) has a similar receptor-binding domain structure as SARS-CoV which suggests COVID-19 (SARS-CoV-2) uses ACE2 receptor in humans for infection.
- COVID-19 (SARS-CoV-2) Structure:
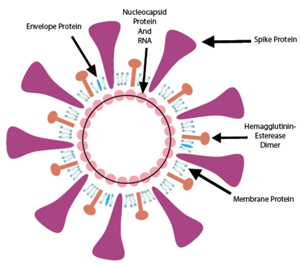
- The structure of COVID-19 (SARS-CoV-2) consists of the following: a spike protein (S), hemagglutinin-esterease dimer (HE), a membrane glycoprotein (M), an envelope protein (E) a nucleoclapid protein (N) and RNA as seen in the figure below.
- Spike protein (S) is heavily glycosylated, utilizes an N-terminal signal sequence to gain access to the ER and mediate attachment to host receptors. It is the largest structure and makes the distinct spikes on the surface of the virus. For most coronaviruses, S protein is cleaved by a host cell furin-like protease into two separate polypeptides S1 and S2.
- RNA is the genome of the virus.
- Nucleocapsid protein (N) binds to RNA in vitro and is heavily phosphorylated. N proteins binds the viral genome in a beads on a string type conformation. This protein likely helps tether the viral genome to replicase-transcriptase complex (RTC), and subsequently package the encapsulated genome into viral particles.
- Envelope protein (E) is found in small quantities in within the virus. It is most likely a transmembrane protein and with ion channel activity. The protein facilitates assembly and release of the virus and has other functions such as ion channel activity. It is not necessary for viral replication but it is for pathogenesis.
- Membrane protein (M) is the most abundant structural protein. It does not contain signal sequence and exists as a dimer in the virion. It may have two different conformations to enable it to promote membrane curvature as well as bind to nucleocapsid.
- Hemagglutinin-esterase dimer protein (HE) is present in a subset of betacoronaviruses. The protein binds sialic acids on surface glycoproteins. The protein activities are thought to enhance S protein-mediated cell entry and virus spread through the mucosa.
7. Covid-19の構造 (ProSci):
- ACE2: angiotensin-coverting enzyme-2; 不活性体であるAng Iを活性体のAng IIに変換する触媒; 喫煙によるこの活性低下があり得る
- glcosylate: グリコシル化、糖化・糖鎖形成する
- ER: endoplasmic reticulum, 細胞の小胞体
- mucosa: 粘膜
- Covid-19 ウイルスの構造:
2019-nCoVとして知られている新型コロナウイルス SARS-CoV-2 は急性呼吸器疾患を引き起こす。2020/3/11にWHOはこのCovid-19をパンデミックと認定した。
- Covid-19は、コウモリ由来のβコロナウイルス属に種類。βコロナウイルスは哺乳類に感染し、人獣共通感染症で、人に重症な呼吸器疾患を起こす。同じ種類のウイルスに、SARSコロナウイルスとMERSコロナウイルスがる。Covid-19は、SARSウイルスとは79% (注: 96%という文献あり)、MERSウイルスとは50%ゲノムが一致している。形体的には、Covid-19はSARS-CoVと同様の受容体結合構造を持ち、人のACE2受容体を利用して感染すると示唆される。
- Covid-19の構造:
スパイク蛋白質 (S); 赤血球凝集素エステラーゼ二量体
(HE); 膜糖蛋白質 (M); エンベロープ蛋白質 (E); 核小体蛋白質 (N); およびRNAである。
- スパイク蛋白質 (S):
高度に糖化しており、N末端シグナルシーケンスを利用してERにアクセスして、ホスト受容体への結合を仲介する。これは最大の構造で、ウイルス表面に明確なスパイクを作る。S蛋白質は、宿主細胞のフリン様プロテアーゼによって2つのポリペプチドS1とS2に切断される。
- このウイルスのゲノムはRNAである。
- ヌクレオカプシド蛋白質(N)は、実験ではRNAと結合し、高度にリン酸化される。N蛋白質は、ストリング型立体構造のビーズのウイルスゲノムに結合する。この蛋白質は、ウイルスゲノムをRTCに結合するのに役立つ。これはウイルス複製には必要ないが、病因となる。
- エンベロープ蛋白質 (E)は、ウイルス内に少量含まれる。それはおそらく膜貫通蛋白質で、イオンチャンネル活性を伴う。それはシグナル配列を含まず、ビリオン二量体として存在する。それはおそらく膜の湾曲を促進し、ヌクレオカプシドへの結合するために2つの異なる形体を持っている可能性がある。
- 赤血球凝集素エステラーゼ二量体 (HE)は、βコロナウイルスのサブセットとして存在する。この蛋白質は、表面の糖蛋白質のシアル酸に結合する。蛋白質の活動は、S 蛋白質を介した細胞への侵入と粘膜を介したウイルスの拡散を促進すると考えられている。
>Top 6. Report from CDC (Centers for Disease Control and Prevention):
- Covid-19 cases in US: CDC recommends:
- Everyone can do their part to help us respond to this emerging public health threat:
- On March 16, the White House announced a program called “15 Days to Slow the Spread,” which is a nationwide effort to slow the spread of COVID-19 through the implementation of social distancing at all levels of society.
- Older people and people with severe chronic conditions should take special precautions because they are at higher risk of developing serious COVID-19 illness.
- If you are a healthcare provider, use your judgment to determine if a patient has signs and symptoms compatible with COVID-19 and whether the patient should be tested. Factors to consider in addition to clinical symptoms may include:
- Does the patient have recent travel from an affected area?
- Has the patient been in close contact with someone with COVID-19 or with patients with pneumonia of unknown cause?
- Does the patient reside in an area where there has been community spread of COVID-19?
- If you are a healthcare provider or a public health responder caring for a COVID-19 patient, please take care of yourself and follow recommended infection control procedures.
- People who get a fever or cough should consider whether they might have COVID-19, depending on where they live, their travel history or other exposures. More than half of the U.S. is seeing some level of community spread of COVID-19. Testing for COVID-19 may be accessed through medical providers or public health departments, but there is no treatment for this virus. Most people have mild illness and are able to recover at home without medical care.
- For people who are ill with COVID-19, but are not sick enough to be hospitalized, please follow CDC guidance on how to reduce the risk of spreading your illness to others. People who are mildly ill with COVID-19 are able to isolate at home during their illness.
- If you have been in China or another affected area or have been exposed to someone sick with COVID-19 in the last 14 days, you will face some limitations on your movement and activity. Please follow instructions during this time. Your cooperation is integral to the ongoing public health response to try to slow spread of this virus.
- Covid-19 Emergence:
- COVID-19 is caused by a coronavirus. Coronaviruses are a large family of viruses that are common in people and many different species of animals, including camels, cattle, cats, and bats. Rarely, animal coronaviruses can infect people and then spread between people such as with MERS-CoV, SARS-CoV, and now with this new virus (named SARS-CoV-2).
- The SARS-CoV-2 virus is a betacoronavirus, like MERS-CoV and SARS-CoV. All three of these viruses have their origins in bats. The sequences from U.S. patients are similar to the one that China initially posted, suggesting a likely single, recent emergence of this virus from an animal reservoir.
- Early on, many of the patients at the epicenter of the outbreak in Wuhan, Hubei Province, China had some link to a large seafood and live animal market, suggesting animal-to-person spread. Later, a growing number of patients reportedly did not have exposure to animal markets, indicating person-to-person spread. Person-to-person spread was subsequently reported outside Hubei and in countries outside China, including in the United States. Some international destinations now have ongoing community spread with the virus that causes COVID-19, as do some parts of the United States. Community spread means some people have been infected and it is not known how or where they became exposed. Learn more about the spread of this newly emerged coronavirus.
- Severity:
- The complete clinical picture with regard to COVID-19 is not fully known. Reported illnesses have ranged from very mild (including some with no reported symptoms) to severe, including illness resulting in death. While information so far suggests that most COVID-19 illness is mild, a reportexternal icon out of China suggests serious illness occurs in 16% of cases. Older people and people of all ages with severe chronic medical conditions — like heart disease, lung disease and diabetes, for example — seem to be at higher risk of developing serious COVID-19 illness. A CDC Morbidity & Mortality Weekly Report that looked at severity of disease among COVID-19 cases in the United States by age group found that 80% of deaths were among adults 65 years and older with the highest percentage of severe outcomes occurring in people 85 years and older.
Learn more about the symptoms associated with COVID-19.
- Covid-19 Pandemic:
- A pandemic is a global outbreak of disease. Pandemics happen when a new virus emerges to infect people and can spread between people sustainably. Because there is little to no pre-existing immunity against the new virus, it spreads worldwide.
- The virus that causes COVID-19 is infecting people and spreading easily from person-to-person. On March 11, the COVID-19 outbreak was characterized as a pandemic by the WHOexternal icon .
- This is the first pandemic known to be caused by a new coronavirus. In the past century, there have been four pandemics caused by the emergence of new influenza viruses. As a result, most research and guidance around pandemics is specific to influenza, but the same premises can be applied to the current COVID-19 pandemic.
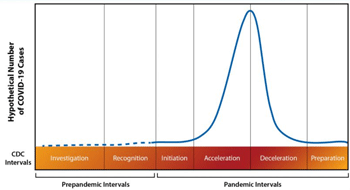
- Pandemics of respiratory disease follow a certain progression outlined in a “Pandemic Intervals Framework.” Pandemics begin with an investigation phase, followed by recognition, initiation, and acceleration phases. The peak of illnesses occurs at the end of the acceleration phase, which is followed by a deceleration phase, during which there is a decrease in illnesses. Different countries can be in different phases of the pandemic at any point in time and different parts of the same country can also be in different phases of a pandemic.
- Risk Assessment:
- Risk depends on characteristics of the virus, including how well it spreads between people; the severity of resulting illness; and the medical or other measures available to control the impact of the virus (for example, vaccines or medications that can treat the illness) and the relative success of these. In the absence of vaccine or treatment medications, nonpharmaceutical interventions become the most important response strategy. These are community interventions that can reduce the impact of disease.
- The risk from COVID-19 to Americans can be broken down into risk of exposure versus risk of serious illness and death.
- Risk of exposure:
- The immediate risk of being exposed to this virus is still low for most Americans, but as the outbreak expands, that risk will increase. Cases of COVID-19 and instances of community spread are being reported in a growing number of states.
- People in places where ongoing community spread of the virus that causes COVID-19 has been reported are at elevated risk of exposure, with the level of risk dependent on the location.
- Healthcare workers caring for patients with COVID-19 are at elevated risk of exposure.
- Close contacts of persons with COVID-19 also are at elevated risk of exposure.
- Travelers returning from affected international locations where community spread is occurring also are at elevated risk of exposure, with level of risk dependent on where they traveled.
- Risk of Severe Illness:
- Early information out of China, where COVID-19 first started, shows that some people are at higher risk of getting very sick from this illness. This includes:
- Older adults, with risk increasing by age.
- People who have serious chronic medical conditions like:
- Heart disease
- Diabetes
- Lung disease
- CDC has developed guidance to help in the risk assessment and management of people with potential exposures to COVID-19.
- What may happen:
- More cases of COVID-19 are likely to be identified in the United States in the coming days, including more instances of community spread. CDC expects that widespread transmission of COVID-19 in the United States will occur. In the coming months, most of the U.S. population will be exposed to this virus.
- Widespread transmission of COVID-19 could translate into large numbers of people needing medical care at the same time.
- Schools, childcare centers, and workplaces, may experience more absenteeism. Mass gatherings may be sparsely attended or postponed.
- Public health and healthcare systems may become overloaded, with elevated rates of hospitalizations and deaths.
- Other critical infrastructure, such as law enforcement, emergency medical services, and sectors of the transportation industry may also be affected. Healthcare providers and hospitals may be overwhelmed.
- At this time, there is no vaccine to protect against COVID-19 and no medications approved to treat it. Nonpharmaceutical interventions will be the most important response strategy to try to delay the spread of the virus and reduce the impact of disease.
- CDC Response:
- Global efforts at this time are focused concurrently on lessening the spread and impact of this virus. The federal government is working closely with state, local, tribal, and territorial partners, as well as public health partners, to respond to this public health threat.
- Highlights of CDC's response:
- CDC established a COVID-19 Incident Management System on January 7, 2020. On January 21, CDC activated its Emergency Operations Center to better provide ongoing support to the COVID-19 response.
- The U.S. government has taken unprecedented steps with respect to travel in response to the growing public health threat posed by this new coronavirus:
- Foreign nationals who have been in China, Iran, the United Kingdom, Ireland and any one of the 26 European countries in the Schengen Area within the past 14 days cannot enter the United States.
- U.S. citizens, residents, and their immediate family members who have been any one of those countries within in the past 14 days can enter the United States, but they are subject to health monitoring and possible quarantine for up to 14 days.
- People at higher risk of serious COVID-19 illness avoid cruise travel and non-essential air travel.
- CDC has issued additional specific travel guidance related to COVID-19.
- CDC has issued clinical guidance, including:
- Clinical Guidance for Management of Patients with Confirmed Coronavirus Disease (COVID-19).
- Infection Prevention and Control Recommendations for Patients, including guidance on the use of personal protective equipment (PPE) during a shortage.
- CDC also has issued guidance for other settings, including:
- Preparing for COVID-19: Long-term Care Facilities, Nursing Homes
- Discontinuation of Home Isolation for Persons with COVID-19
- CDC has deployed multidisciplinary teams to support state health departments in case identification, contact tracing, clinical management, and public communications.
- CDC has worked with federal partners to support the safe return of Americans overseas who have been affected by COVID-19.
- An important part of CDC’s role during a public health emergency is to develop a test for the pathogen and equip state and local public health labs with testing capacity.
- CDC developed an rRT-PCR test to diagnose COVID-19.
- As of the evening of March 17, 89 state and local public health labs in 50 states, the District of Columbia, Guam, and Puerto Rico have successfully verified and are currently using CDC COVID-19 diagnostic tests.
- Commercial manufacturers are now producing their own tests.
- CDC has grown the COVID-19 virus in cell culture, which is necessary for further studies, including for additional genetic characterization. The cell-grown virus was sent to NIH’s BEI Resources Repositoryexternal icon for use by the broad scientific community.
- CDC also is developing a serology test for COVID-19.
- Other Available Resources:
- The following resources are available with information on COVID-19
- World Health Organization, Coronavirusexternal icon
6. CDCからの報告:
- AIIR: 空気感染隔離室
- PPE: 個人用防護具
- RT-PCR: Rverse Transcription-Polymerase Chain Reaction
- Serelogy: 血清学 <blood serum 血清
- Response to pandemic: typicallly follow a patter and can be divided into intervals:
- Prepandemic intervals: 感染爆発前
- Investigation: 調査
- Recognition: 認知
- Pandemic intervals: 感染爆発期
- Initiation: 初期
- Acceleration: 感染加速期
- Deceleration: 感染減速期
- Preparation: 収束準備
- Covid-19感染に関するCDCの勧告:
- 各人がやるべきこと:
- 3/16に米国ホワイトハウスは'15日間感染スロー対策'を発表し、社会的距離を取るように指示
- 高齢者は、特にリスクが高いので注意が必要
- 医療従事者は患者の症状によって処理を判断する。その症状は
- 感染地域に旅行したか
- Covid-19患者と濃密接触したか
- Covid-19汚染地域に居住しているか
- 医療従事者は、自身に対し適切な感染予防をとる。
- 米国の半分以上の地域は、あるレベルでCovid-19で感染している。このウイルスに対してはまだ適切な治療法がない。多くの患者は軽症で医療機関に行かなくても自宅で治癒できる。
- 感染者で、入院するまでもない場合は、CDCのガイドに従って他人にうつさないようにする。軽症の場合は自宅隔離すべきである。
- 過去14日以内に、中国その他の感染地域に滞在していた場合は、移動・行動制限に従う。
- Covid-19の出現:
- Covid-19はコロナウイルスで、人間や各種動物 (駱駝、牛、猫、コウモリ等)に通常に感染する種類のウイルスであり、MERS-CoVやSARS-CoVと同様に、人から人へ感染し、SARS-CoV-2と名付けられた。
- SARS-CoV-2ウイルスはMERS-CoVやSARS-CoVと同じβコロナウイルスで、その3つの感染源はコウモリである。米国の患者と中国の患者のウイルス遺伝子配列は同じなので感染源は同じ動物からであると示唆される。
- 当初は中国河北省武漢市から感染が広がった。そこには動物や海産物市場があり、そこの動物から人へ感染したものと見られる。その後多くの感染者が発生したので人から人への感染が中国以外にも拡大した。多くの地域に拡大したので、感染源が特定できなくなった。
- 重症化:
- 臨床に関する全体像はまだ明らかではない。ごく軽症から死亡に至るまである。多くの場合は軽症だが、中国の事例では16%の患者は重症化する。高齢者でかつ既往症 (心臓病、火病、糖尿病等)の患者はハイリスクである。米国での死亡者の80%は65歳以上で、85歳以上は特にハイリスクである。
- パンデミック:
- 新型ウイルスに対する既存の抗体保有者はいないので、世界的に感染拡大する。
- WHOは3/11にパンデミックを宣言。
- 20世紀に4回パンデミックがあった。
- パンデミック拡大には、各段階がある。感染者のピークは加速期の最後に発生。パンデミックの様相は各国各地域で異なる。
- リスク評価:
- リスクは、人々の間でどのように感染が拡大するか; 症状の軽重;ウイルスに対する治療方針等。ワクチンや治療法が確立していない現状では、非医薬品以外の方法で症状を抑えるしかない。
- Covid-19のリスクは以下に分類:
- 感染リスク影響度:
- 当初はリスク影響度は低いが、一体アウトブレイクするとリスクは急増。
- リスクレベルは場所に依存する。
- 医療従事者のリスクレベルは高い。
- 濃厚接触者のリスクレベルは高い
- 感染地域への旅行者のリスクは高い。
- 重症化リスク:
- 一部の感染者のリスクは高い。高齢者は年齢とともにリスク増大
- 慢性的重症患者 (心臓病、糖尿病、肺病)のリスクは高い。
- CDCは、Covid−19感染リスク評価と管理のガイダンスを公表した。
- 今後の可能性:
- 米国での完成者は数日の単位で増加。今後全米での感染拡大の可能性がある。数ヶ月以内に米国人国の多くが感染する可能性がある。
- このような大量感染によって、膨大な人々が同時に医療サービスが必要となる。
- 学校、ケアセンター、職場等の閉鎖が必要となる。大勢の集会の禁止・延期。
- 医療機関の過剰化、入院率・死亡率の増加
- 法的強制、緊急医療サービス、輸送手段に影響。医療提供能力の過剰化。
- 抗Covid-19ワクチンや承認薬がない。非医薬療法でウイルスの感染や病状悪化の防止を図るしかない。
- CDCの対応:
- 国際連携での感染減少の努力は必須。連邦政府は州・各地域・各民族集団と連携して公衆衛生への危機対応が必要。
- 特に留意事項:
- CDCは、2020/1/7に、Covid-19対策管理システムを公表。1/21に、緊急オペレーションセンタを立ち上げてCovid-19対策を実施。
- 米国政府は、公衆衛生での増大する危機に対する前例のない政策を採用。
- 過去14日以内に、中国、イラン、英国、欧州26カ国に滞在した外国人は米国への入国禁止。
- 米国市民・永住者・その家族は、過去14以内にこれらの国々に滞在していても米国への入国は可能。但し、健康観察および14日間までの隔離が条件。
- Covid-19高リスクの人は、クルーズ船および必須でない航空機の利用を避ける。
- CDCは、別途旅行ガイドを発行。
- CDCは以下の診療ガイドを公表した。
- Covid-19患者に対する診察ガイド
- 個人用感染防御具(PPE)使用を含む感染防止・管理法を公表。
- さらに長期ケア、自宅療養について設備対策
- Covid-19感染者の自宅隔離の中止
- CDCは、学際を越えたチーム編成で、感染同定、感染追跡、診療管理、情報提供を実施。
- CDCは、海外での米国人感染者の安全帰国を連邦職員と連携して支援。
- CDCは、ウイルス検査・地域の医療研究機関の検査能力での支援の役割。特に
- Covid-19診断のrRT-PCR検査
- 3/17段階では、89の州・地域の公衆衛生研究機関で、Covid-19診断試験を検証した。
- 関連業界も現在、独自の検査法を生産中。
- 細胞内増殖ウイルスはNIHの研究所に送り、さらに研究中。
- CRDは、Covid-19の血清学検査を実施中。
- そのほかCovid-19関連情報として、WHOの情報参照。
>Top 7. An address from Merkel:
- An address to the nation by Federal Chancellor Merkel (19/Mar./2020):
- Fellow citizens,
The coronavirus is changing daily life in our country dramatically at the present. Our idea of normality, of public life, social togetherness - all of this is being put to the test as never before. Millions of you cannot go to work, your children cannot go to school or kindergarten, theatres and cinemas and shops are closed, and, perhaps what is most difficult, we all miss social encounters that we otherwise take for granted. Of course, each of us has many questions and concerns in a situation like this, about the days ahead.
- I’m addressing you in this unconventional way today because I want to tell you what guides me as Federal Chancellor and all my colleagues in the Federal Government in this situation. This is part of what open democracy is about: that we make political decisions transparent and explain them. That we justify and communicate our actions as best we can, so that people are able to understand them. I firmly believe that we will pass this test if all citizens genuinely see this as THEIR task.
- Allow me therefore to say that this is serious. Please also take this seriously. Since German reunification, no, since the Second World War, there has not been a challenge for our country in which action in a spirit of solidarity on our part was so important.
- I would like explain where we currently stand in this epidemic and what the Federal Government and the state levels are doing to protect everyone in our community and to limit the economic, social and cultural fallout. However, I also want to tell you why all of you are needed here, and what each and every individual can do to help.
- As far as the epidemic is concerned – and everything I tell you about this comes from the Federal Government’s ongoing consultations with the experts from the Robert Koch Institute and other scientists and virologists: the most intensive research is being conducted around the world, but there is still neither a way to treat the coronavirus, nor is there a vaccine.
- As long as this is the case – and this is what is guiding all of our actions – then only one thing matters, namely that we slow the spread of the virus, flatten the curve over the course of several months and buy time. Time in which the research community can develop a medicine and vaccine. But, above all, time to allow those who fall ill to receive the best possible treatment.
- Germany has an excellent healthcare system, perhaps one of the best in the world. We can take solace in this. But our hospitals would also be completely overwhelmed if, in the shortest space of time, too many patients were admitted, suffering severe symptoms as a result of the virus.
- These are not just abstract numbers in statistics, but this is about a father or grandfather, a mother or grandmother, a partner – this is about people. And we are a community in which each life and each person counts.
- I would like first of all to address all those who as doctors, nurses or in a different capacity work in our hospitals and in our healthcare system in general. You are on the front lines of this fight for us. You are the first to see the sick and to see how severe the symptoms of the virus can sometimes be. And, day in, day out, you keep going back to work and are there to help people. You are doing tremendous work, and I would like to thank you from the bottom of my heart.
- So, our aim is to slow the virus down as it makes its way through Germany. And we must, and this is absolutely vital, focus our attention on one thing above all else, namely powering down public life as far as possible. With reason and a sense of proportion, of course, since the state will continue to function. It goes without saying that supply chains will continue to be guaranteed, and we want to keep as much economic activity going as possible.
- But we must now reduce everything that could put people at risk, everything that could harm not only individuals, but also the community. We must limit the risk of one person infecting another as much as we possibly can.
- I know how dramatic the restrictions already are: no events, no trade fairs, no concerts any more, and, for the time being, also no school, no university, no kindergarten, no more playing at the playground. I know how invasive the closures that the Federation and the Länder have agreed to are in our lives, and also in terms of how we see ourselves as a democracy. These are restrictions, the likes of which the Federal Republic has never seen before.
- Allow me to assure you that, for someone like me, for whom the freedom of travel and the freedom of movement were a hard-fought right, such restrictions can only be justified if they are absolutely imperative. These should never be put in place lightly in a democracy and should only be temporary. - But they are vital at the moment in order to save lives.
- This is why, since the beginning of the week, more intensive border controls and restrictions on entry for a number of our most important neighbouring countries have been in force. Things are already very difficult for the economy, for major companies, and also for small businesses, for shops, restaurants and freelancers. Things will get even more difficult in the weeks to come.
- I assure you that the Federal Government is doing everything that it can to cushion the economic impact - and, above all, to safeguard jobs. We can and we will do whatever it takes in order to help our companies and their employees get through this most difficult time.
- And everyone can rest assured that the food supply is guaranteed at all times, and that if supermarket shelves happen to be empty on one day, they will be filled again on the next. I want to tell everyone going to the supermarket that bulk-buying makes sense; it always has. But only within reason. Panic buying, as if there’s no tomorrow, is pointless and, at the end of the day, shows a complete lack of solidarity.
- And allow me to express my thanks to those who are too seldom thanked. Those working as supermarket cashiers or restocking shelves, who are currently doing one of the most difficult jobs that there are at the moment. Thank you for being there for your fellow citizens and for keeping us all going.
- Let me talk now about what I believe is most urgent today. All measures taken by the state would come to nothing if we were to fail to use the most effective means for preventing the virus from spreading too rapidly – and that is we ourselves. As indiscriminately as each one of us can be affected by the virus, each and every one of us must help. First and foremost, by taking seriously what matters today. Not panicking, but also not thinking for a single moment that he or she doesn’t matter after all. No one is expendable. Everyone counts, and we need a collective effort.
- That is the message an epidemic brings home – how vulnerable we all are, how much we depend on the considerate behaviour of others and, ultimately, how, through joint action, we can protect ourselves and offer one another encouragement and support.
- Every individual counts. We are not condemned to accept the spread of this virus as an inevitable fact of life. We have the means to fight it. We must be considerate and keep a safe distance from one another. Virologists are giving us clear advice: no more handshakes, we must wash our hands thoroughly and often, and we must keep at least one and a half metre’s distance between ourselves and others. Ideally, we should avoid all contact with the elderly, because they are particularly at risk.
- I know that this is asking a great deal of us. Especially when times are hard, we want to be close to one another. We show affection by staying close, and by reaching out to each other. But at this time, we must do the exact opposite. Every single one of us must understand that, right now, the only way to show we care is by keeping our distance.
- A well-meant visit or a trip that is not essential can spread infection and really should not take place right now. There is a reason why experts say that grandparents and grandchildren should not come into contact with each other right now. Everyone who avoids unnecessary encounters helps all those who are in hospitals providing care to more and more people each day. So that is how we will save lives. This will be difficult for many, and it will also be important not to abandon anyone and to take care of all those who need a dose of cheer and encouragement. As families, and as a society, we will find other ways to help each other.
- Even now, we have come up with many creative ideas for standing up to this virus and its impact on society. Even now, grandchildren are recording podcasts for their grandparents, letting them know they are not alone. We all must discover how we can show affection and express friendship. We are staying in touch via Skype, phone, email, and maybe also by writing old-fashioned letters. The post, after all, is being delivered. We’re hearing about beautiful examples of neighbours helping one another. People are assisting the elderly who cannot themselves go shopping. I am certain there’s plenty more we can do. We will prove, as a community, that we will not abandon one another.
- I therefore urge you to abide by the rules that will remain in place for the time being. The government will constantly reassess what measures can be adjusted and also what further measures may still be necessary. This is a developing situation, and we will ensure that we continue to learn from it so that we can adjust our thinking and deploy new instruments at any time. If we do so, then we will explain our reasons once again. Therefore, I call on you to not believe any rumours, but rather only the official messages that we will always translate into many languages.
- We are a democracy. We thrive not because we are forced to do something, but because we share knowledge and encourage active participation. This is a historic task, and it can only be mastered if we face it together. I have absolutely no doubt that we will overcome this crisis. But how many victims will it claim? How many loved ones will we lose? The answer, to a great extent, lies in our hands. Right now, we can take decisive action all together. We can accept these current limitations and support one another.
- The situation is serious, and the outcome uncertain.
Our success will also largely depend on how disciplined each and every one of us is in following the rules. Even though this is something we have never experienced before, we must show that we can act warm-heartedly and rationally – and thereby save lives. It is up to each and every one of us to do so, without any exception. Take good care of yourself and your loved ones. Thank you.
7. 独メルケル首相声明:
- 独連邦メルケル首相の国民向け声明 (2020/3/19):
- 親愛なる市民各位:
現在、コロナウイルスは我が国の日常を劇的に変えています。我々の正当性、公共性格、社会的一体性の考えの全てが、かつてないほど試されています。何百万もの人々は働きに行くことができず、子どもたちは学校や幼稚園に行けず、映画館や店舗は閉鎖されており、もっと困難なことには、当然のことである社会的な出会いを失っていることです。このような状態に対して多くの疑問や関心がそれぞれにあると思います。
- 本日は、型破りの方法で、連邦首相として、連邦政府の全ての同僚として、必要とされることをお伝えしたい。これはオープンデモクラシーとしての一部分としても、政治的な決定を透明度を持って説明すべきことだと思います。我々の行動を正当化して伝達することは我々ができる最善のことであり、それ故、人々はその行動を理解することができるからです。全ての市民がこれを自分の役割だとみなすならば、このテストに合格できると私は信じています。
- まず、これは深刻であると言わざるをえません。ですから、これを真剣に受け止めて下さい。独の統一、いや第二次大戦以降で、我が国にとって連帯の精神で行動することがこれほど重要であったことはありません。
- 我々は、現在この感染流行にどこで立ち向かっているのか、また連邦と州政府が我々のコミュニティの全ての人々を保護し、経済的・社会的・文化的な影響を制限するのは何のためかを説明したと思います。さらに、全ての人がここで必要とされる理由を一人ひとりが何を支援できるかについてもお話します。
- 感染流行に関して、これから話すことは、Robet Koch 研究所他の専門家やウイルス学者と連邦政府との継続的な協議に基づくものです。世界では集中的な研究が行われていますが、現在の所、まだコロナウイルスに対する治療法やワクチンが開発されていません。
- 現状このような段階で、我々の全ての行動を導かなければならない中で、我々が取るべき方法は、まずウイルスの感染を遅らせることで、それによって感染カーブを何ヶ月間に亘って平坦化することで時間を稼ぐことであります。その時間によって、研究分野では治療法とワクチンを開発することが可能となります。それは感染者に対して最善の処置を施すことが可能となる時間でもあります。
- 独には優秀な、おそらく世界で最善の一つと言える医療制度があります。それは安心材料ではありますが、もし短期間に非常に多数の患者が押し寄せるとしたら、我々の病院は完全に過剰状態となり、ウイルスの結果、重症化した患者に圧倒されることになります。
- これは単に統計上の抽象的な数字ではありません。これは父・祖父・母・祖母・配偶者や人々に関することです。それは各々の生命と人間としてカウントするコミュニティに関わることなのです。
- まず第一に、医療現場にいる医師・看護師・その他医療機関で働いている全ての人達に着目したいです。あなた達はこの戦いの最前線にいて、最初にこの病気と出会い、このウイルスによる症状が時にはどれほど深刻になるかを見つけてきました。そして連日、あなたはその仕事に戻り続け、人々を助けるためにそこにいるのです。実に大変な仕事をしていることに、心から感謝を申し上げます。
- 我々の目的は、独においてのウイルス感染を遅延させることです。それは、我々にとって絶対不可欠なことであり、何よりも我々が注力しなければならないことは、可能な限り我々の公共生活をパワーダウンすることであります。もちろん理性と均衡の感覚を持って、国家は機能し続けることになります。言うまでもありませんが、サプライチェーンは今後も保証されることになるし、可能な限り経済活動も継続して行きたいと思います。
- しかし、今我々は、人々を危険に晒す全ての可能性、個人だけでなくコミュニティを害する全ての可能性を縮減しなければなりません。我々は、一人の人間が他人を感染されるリスクを極力制限しなければならないのです。
- 今、どれほど劇的な制限が行われているか私は知っています。イベント、見本市、コンサートは当分の間なく、また学校・大学・幼稚園・遊び場もなくなっています。連邦と州が合意したこれらの封鎖が、我々の生活の中で、どれほど侵略的なものであるか、同時に我々自身が民主主義としてこれをどう捉えているかについても、私は認識しています。これらの制限は、連邦共和国として今まで見たこともないものなのです。
- 私のように、旅行と移動の自由求めて強く戦ってきた人たちにとって、このような制限は、絶対に不可欠である場合のみ正当化できるということをまず許して下さい。これらは民主主義では決して軽々に置かれるべきことでなく、一時的であるべきことです。しかし、それは生命を救うために今は不可欠なのです。
- これは、今週初めより、多くの重要な近隣諸国との国境管理と入国制限が施行されている理由でもあります。事態は、経済、主要企業、小企業、店舗、レストラン、フリーランサーにとってすでに非常に厳しいことになっている。事態は、今後数週間でさらに困難になると思われます。
- 連邦政府は、経済的な影響を緩和するために、何よりも仕事を守るためにできる限りのことを実行していることを約束します。我々の会社や従業員がこの最も困難な時期を乗り越えるのを支援するため、我々はあるゆることを行います。
- なお、食料供給は常に保証されており、ある日スーパーマーケットの棚が空になっても、翌日には再び満杯になることで誰もが安心できるようにします。全ての人に申し上げたいことは、スーパーマーケットで大量購入は理にかなっており、それは常にそうかも知れないとは思います。しかし、合理的な範囲を越えたパニック状態での購入は、あたかも明日がないかのようで無意味であり、それは結局、連帯が完全に欠如していることになります。
- 普段あまり感謝されない方々に,私として感謝の意を評したいです。それはスーパーマーケットのレジ係や在庫の補充をしている人達です。彼らは、現在、最も困難な仕事の一つを行っています。仲間の市民のために、その場所にいて我々全員を助け続けてくれているのです。
- 今日、何が最も緊急な課題であるかを述べます。ウイルスが急激に感染するのを防ぐために最も効果的な方法を採ることができなかったとしたら、国にとってあらゆる措置は意味がなくなることになります。それは我々自身の問題です。我々一人ひとりがウイルスから無差別の影響を受ける可能性があるのと同様に、我々は一人ひとりを助けなければならないのです。何よりも、今日の事態の重要性を真剣に受け止める必要があります。慌てる必要はありませんが、それが重要でないといささかも考えてはならなりません。誰もが消耗品のように代替えがきかないのです。誰もが重要であり、我々は共同の努力を必要としているのです。
- 伝染病が、家庭にもたらすメッセージとは、即ち、我々全員がいかに脆弱であるか、いかに他人の思慮ある行動に依存しているか、そして共同行動を通じて、いかに我々は自身を守り、互いに励ましと支援を提供するかということです。
- 全ての個人が重要なのです。我々は、このウイルスの蔓延を防げられないことを事実として受け入れることで非難はされません。しかし、我々にはそれと戦う手段があります。我々は思いやりがあると同時に、互いに安全な距離を保つ必要があります。ウイルス学者の忠告は明確です。握手をするな、頻繁に手洗いをせよ、他人との距離を1.5m空けよということです。高齢者は特にリスクが高いので、理想的には全ての接触を避ける必要があります。
- 我々には多くのことが求められている。特に、現状が厳しい時には、互いに近づきたくなります。親密に近づいて相互に手を差し伸べたいと思います。しかし、現時点では、我々は全く逆のことをしなければならないのです。今、我々が気遣うべきことは、互いの距離を保つことであることを理解する必要があります。
- 善意の訪問または必須でない旅行は感染を拡大する可能性があるので、今はそれをやめるべきです。専門家が、今は、祖父母と孫が会うべきではないというのには理由があるのです。不必要な出会いを避けることによって、結果的に、病院にいる全てスタッフが多くの人を毎日ケアすることを助けることに通じます。それが命を救う方法なのです。これは多くの人にとって困難なことであり、誰かを捨てることなく、歓声と激励を必要とする人達をケアすることが必要なのです。家族としても、社会としても、互いに助け合う他の方法も見つけて行く必要があります。
- 今までも、このウイルスや社会への影響に立ち向かうために独創的なアイデアを考え出してきました。孫は、祖父母のためにポッドキャストを録音しており、一人でないことを伝えています。我々は皆、愛情を示し、友情を表現する方法を発見する必要があります。我々は、Skype、電話、電子メール、昔ながらの手紙を書くことで連絡を取り合っています。買い物に行けないお年寄りを手伝っています。他にも我々にできることは沢山あると思います。我々はコミュニティとして互いに見捨てないことを約束していきましょう。
- 結論として、当面はそのルールを守るよう要請します。政府は常に取るべき対策を調整し、さらに必要な対策はなにかを再評価していきます。まだ道半ばであり、我々は引き続き教訓を得て、我々の考えを調整し、新たな手段を投入していけるようにしていきます。その場合は、再度その理由を説明します。従って噂を信ずるのではなく、常に多くの言語に翻訳される公的なメッセージのみを信ずるようにお願いします。
- 我々は民主主義であります。我々はなにかを強制されてするのではなく、知識を共有し、積極的に参加することを奨励されます。これは歴史的な任務であり、それに直面することで初めて習得できます。私は、今回の危機を乗り越えることに対しての疑念は一切ありません。しかし何人の犠牲者が出てくることになるのか、どれほど多くの愛する人達を別れなければならないのか、その答えは、ある程度、我々の手中にかかっています。今や、我々は一丸となって決断を下そうではありませんか。我々は、現在の制限を受け入れ、互いに助け合うことができるのです。
- 状況は深刻で、その結果の見通しは不確実であります。我々が成功するかどうかは、我々一人ひとりがルールを遵守するかどうかにかかっています。これは我々は今まで経験したことがないが、我々は心温かく合理的に行動できることを示し、ともかく命を救う必要があります。それは例外はなく、我々の一人ひとりの責任でもあります。あなた自身を、そしてあなたの愛する人達を大切にしてください。ありがとうございます。
>Top 8. Covid-19 therapeutic candidate:
- Avigan, anti-influenza virus activator:
- When ribose is added to avigan, whose structure resembles that of AICAR; inosine is synthesized from AICAR and guanosine from inosine in vivo.
- AICAR is a precursor to inosine, which is a precursor to guanosine and adenosine, which are used for RNA. The viral RNA-dependent RNA synthase (RdRp) mistakenly incorporates avigan into the elongating viral RNA with guanosine or adenosine, which consequently stops RNA synthesis.
8. Covid-19治療薬候補:
- AICAR: 5-aminoimidazole-4-carboxamide-1-β-D
-ribofuranoside; inosine, then guanosine is sy
- Structure of Avigan (Favipravir):
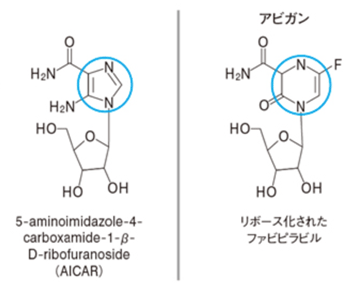
Comment
- ウイルスに関する疑問
- ウイルス (Covid-19)の生存期間:
- NIHの報告では、ウイルスは空気中エアロゾル内で数時間滞在し、段ボール表面では24時間、プラスティックやステンレス表面では2-3日生存できるという。ウイルスはこの生存のエネルギーをどう補給しているのか? あるいは死滅する原因は、UV放射線や熱や湿気などによる何らかの化学変化によるウイルスの持っている蛋白真の変異かあるはそれ自身のエネルギー枯渇によるものか、あるいはウイルスの遺伝子自身に寿命があるのか?
- ウイルスのエネルギー源:
- 宿主細胞への侵入プロセスなどのエネルギーはどこから補給されるのか。侵入時点では、まだ宿主のエネルギーを横取りして利用できないのではないか。
- ウイルスは、宿主に侵入するまでは、非生物、侵入後は生物的なふるまいをすると思われるが、その切替の司令はどのタイミングなのか。
- ウイルスの生存戦略:
- 宿主の発熱や病気の重篤化は、ウイルスの生存戦略によって有害と思う。なぜ、そのような癌細胞的な振る舞いをするのか。
- ウイルスは、生存戦略から言って、健康で発熱も重篤化もしないで粛々と増殖を手助けしてくれる健康な若者を好むと思うが、宿主の選考はあるのか。あるいは、宿主の免疫能力とのトレードオフなのか。
- 自然抗体を持つ宿主が増えると、その分、ウイルスにとって増殖の機会がなくなるので、ウイルスの生存戦略の見直しが迫られると思うが、それは変異など偶然性に依存するのか、それとも長期的戦略があってしばらく冬眠状態になるということか? (生命誕生の頃からウイルスと他生物との共存関係が地球上で維持されてきた歴史もあるので)
- ウイルスのルーツ:
- 真核生物の核は、そのルーツは、ある種のウイルスだったという説はその後どうなったのか。その説では、核とウイルスとは、細胞組織を有する既得権力と、細胞組織をもたない新規勢力との闘争ということになるのか、それとも相互に好敵手、古い友人、相思相愛の関係いずれなのか?
What is Virus? |
Novel Coronavirus Disease (Covid-19) |
Cat: SCI |
Reports from WHO, ECDC, CDC, and ProSci |
20406u |
Title |
Novel Coronavirus Disease 2019 (Covid-19) |
新型コロナウイルス (Covid-19) |
Index |
||
Tag |
; 2.4 vs 1.0; 14days; ACE2; Aetiology; Afebrile; Asymptomatic; CFR; ECMO; Incubation period; Infectivity; ; NIV; Pandemic; PPE; Prognosis; RCT; Respiratory tract; SARS-CoV-2; Severity; TESSy; Viral load; Viral RNA; Vital shedding; | |
Data |
||
Why |
|
|
Original resume |
Remarks |
|
>Top 0. WHO declared pandemic
|
0. WHOパンデミック宣言:
|
Original resume |
Remarks |
|
>Top 1. Pandemic Covid-19: from ECDC report (12 March 2020)
|
1. パンデミック Covid-19 (ECDC報告):
|
>Top 2. Symptom of the cases (ECDC):
|
1. 感染者の症状 (ECDC報告):
|
>Top 3. Outbreak stages: Annex: Scenarios to describe progression of COVID-19 outbreaks
|
3. 感染爆破の諸段階:
|
>Top 4. Advices from WHO: Myth busters
|
6. WHOからの勧告:
|
>Top 5. Structiure of Covid-19 (ProSci)
|
7. Covid-19の構造 (ProSci):
|
>Top 6. Report from CDC (Centers for Disease Control and Prevention):
|
6. CDCからの報告:
|
>Top 7. An address from Merkel:
|
7. 独メルケル首相声明:
|
>Top 8. Covid-19 therapeutic candidate:
|
8. Covid-19治療薬候補:
|
Comment |
|
|